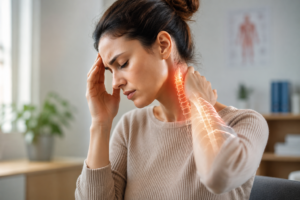
Executive Summary: Urinary incontinence (involuntary leakage of urine) often causes embarrassment, anxiety, and a reduced quality of life. But in addition to physical factors (pregnancy, age, injury), stress, anxiety, fear, and embarrassment play a significant role. These emotions can tense the muscles—especially the pelvic floor—and contribute to symptoms. Our team at the health center in Palma de Mallorca explores how emotions become “embodied” in the body[1] and addresses incontinence from a holistic perspective. Below, we define the types of incontinence, review how stress and the mind influence it, discuss warning signs not to ignore, and outline practical strategies (relaxation, physical therapy, therapy, exercises) that can help restore well-being.
What is urinary incontinence? Definition and types
Urinary incontinence is the involuntary loss of urine due to an inability to control the bladder[2]. It is not a disease in itself, but rather a symptom with many possible causes. Incontinence can affect anyone (it is more common in women) and ranges from occasional leakage when coughing to frequent, urgent leaks. As the Mayo Clinic summarizes: “Urinary incontinence… is a common problem that often causes embarrassment”[2]. The main types of incontinence are:
- Stress incontinence: Urine leakage caused by abdominal pressure (coughing, sneezing, laughing, or lifting heavy objects)[3]. It is most common in women, often following pregnancy or due to weakened pelvic floor muscles[4][5].
- Urge incontinence: Urine leakage caused by a sudden, intense urge to urinate, before reaching the bathroom in time[6]. It can occur with an overactive or irritated bladder and is sometimes associated with emotional stress[7][8].
- Overflow incontinence: Frequent leakage of urine because the bladder does not empty completely[9]. It usually occurs when there is a urinary obstruction or a failure to empty the bladder.
- Functional incontinence: This occurs when a person is unable to reach the bathroom in time due to physical or mental health issues (such as arthritis or dementia)[10].
- Mixed incontinence: A combination of stress and urge incontinence. It is common in women who experience both types[11].
Below is a comparison table of these types:
| Type of incontinence | Features | Common causes | Initial handling |
| Strenuous | Air escapes when you cough, sneeze, laugh, or exercise. | Weak pelvic floor (pregnancy, childbirth, obesity)[4]. Chronic cough (smoking). | Kegel exercises and pelvic floor physical therapy. Weight loss and reducing abdominal pressure. Avoid dry coughing. |
| Urgent | Urinary incontinence following a sudden, intense urge to urinate. | Overactive bladder, cystitis, neurological damage. Sometimes emotional stress[8] or anxiety. | Bladder training (delaying urination), reducing caffeine and diuretics, and antibiotics if there is an infection. Medications to relax the bladder. |
| By overflow | Continuous or frequent dripping due to incomplete emptying. | Urinary obstruction (enlarged prostate, tumor, stones)[12], neurological damage, atonic bladder. | Scheduled bladder emptying (double voiding), intermittent catheterization, treat the underlying cause of the obstruction. |
| Functional | Inability to get to the bathroom (due to mobility or cognitive issues). | Joint problems, neurological issues, dementia, lack of accessibility. | Adapting the environment (accessible restroom), regular bathroom schedules, behavioral training, and external assistance. |
| Combined (effort + urgency) | Symptoms of straining and urgency together. | A combination of the above causes. | Combine different approaches: physical therapy, bladder training, and medication as needed. |
Emotions and Somatization in Incontinence
Stress and anxiety. Chronic stress triggers the “fight-or-flight” response: it releases adrenaline and cortisol, increasing overall muscle tension[13]. In this state, it is common for the pelvic floor muscles to contract unconsciously[13]. Over time, this stiffness impairs normal function: urinary urgency or incontinence may develop. In fact, one study found that women with high levels of anxiety are up to twice as likely to develop pelvic disorders (such as incontinence)[14]. It is a vicious cycle: “prolonged stress can tense the muscles so much that it ends up affecting the pelvic floor and causing incontinence. That same loss of control can lead to more anxiety”[15].
Shame and fear. Incontinence often causes shame. According to a recent study, women with incontinence fear experiencing an embarrassing episode in public[16]. This increases anxiety and can lead to isolation. As researchers note, “incontinence is often surrounded by stigmas and myths, and requires a comprehensive understanding… High levels of anxiety and depression are associated with poorer mental well-being in women with incontinence”[17]. Undoubtedly, avoiding discussion of the problem often makes the situation worse. For this reason, our team encourages breaking the taboo: most cases can improve with treatment[18].
Somatization. When negative emotions (anxiety, stress, fear) manifest in the body without a clear physical cause, we refer to psychosomatic symptoms. Although the origin is sometimes difficult to pinpoint, one sign is that the discomfort appears or worsens with stress and changes in nature without a medical explanation. In these situations, the person is not faking their symptoms; the pain or discomfort they feel is real[19]. In the context of incontinence, the body “speaks” through muscle spasms or urgency under emotional pressure. In short: recognizing that stress can cause physical symptoms allows us to address them before they lead to more serious complications.

Figure: Practicing meditation or breathing exercises outdoors can reduce physical tension and anxiety, which contribute to incontinence[20]Evidence suggests that relaxation training reduces pelvic floor stiffness and, consequently, episodes of stress-related urinary leakage.
Muscle tension and the pelvic floor
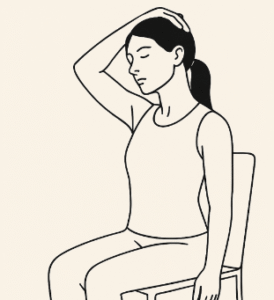
The pelvic floor is the group of muscles that supports the bladder and helps control urination. When these muscles are tense or weakened, they lose their effectiveness. Intense emotions (fear, anger, anxiety) cause automatic muscle tension, even in deep regions of the body[1]. Studies show that in response to highly emotionally charged stimuli, tension is activated in areas such as the jaw, diaphragm, neck, and also in the pelvic floor[1]. If this emotional tension persists over time, the pelvic muscles can become stiff, causing pain, and leading to urinary urgency or incontinence[13][1].
The connection works both ways. As one expert explains: “Anxiety and the pelvic floor share a silent connection… stress damages the pelvic floor, and pelvic floor issues (incontinence, prolapse, etc.) lead to more anxiety”[13]. That is why a comprehensive approach is crucial. Techniques that teach how to relax the pelvic floor are key: for example, deep breathing can “release the pelvis” by consciously lowering these muscles[21]. Recent studies confirm that structured mindfulness can improve urge incontinence by breaking this cycle of tension[20].
Warning signs and when to seek medical attention
Don't ignore the signs. You should seek medical help, especially if there are:
- Frequent or unpredictable leakage: Urinary leakage that occurs several times a week or prevents you from leaving the house.
- Pain when urinating or blood in the urine: This could indicate a pelvic infection or disease.
- A daily need to pass large amounts of urine: Frequent pad changes or frequent wetting of underwear.
- Symptoms accompanied by fever, weight loss, or confusion: These may be signs of serious conditions (severe urinary tract infection, neurological cause, etc.).
In addition, as the Mayo Clinic notes, incontinence can affect daily life[22]. If you feel it restricts your activities, limits your social life, or increases your risk of falls (due to rushing to the bathroom), that is a reason to seek medical advice[22]. Remember that you shouldn’t be embarrassed to talk about it: “Most people with incontinence can get help or be cured”[18]. During the consultation, a medical history (including a voiding diary), physical exam, and urinalysis will be performed[23]. These tests help rule out treatable medical causes (infections, stones, benign prostatic hyperplasia, neurological disorders) before focusing on the emotional component. If all organic causes are ruled out, a comprehensive biopsychosocial approach is adopted.
Impact on well-being and relationships
Living with incontinence affects self-esteem and intimacy. Many people feel dirty or feel they have lost control of their bodies, which undermines their confidence. In a relationship, shame can reduce sexual encounters or cause conflicts: one partner may feel rejected by the other’s precautions, and this increases tension. As the women surveyed indicate, shame and fear of public episodes impair mental well-being[16]. In the long term, untreated incontinence can lead to isolation (avoiding going out) and personal frustration. Therefore, it is essential to address not only the symptom but also personal fulfillment and overall health. Good communication with a partner (explaining limitations, seeking solutions together) and psychological support can alleviate the emotional burden. At our center in Palma, we emphasize psychosocial support: integrating sexuality and self-esteem into treatment to promote overall well-being.
Comprehensive clinical evaluation
In cases of persistent incontinence, the first step is a comprehensive medical evaluation. This includes a detailed medical history (onset of symptoms, frequency, triggers), a physical examination, and basic tests: urinalysis (to rule out infection or blood) and a voiding diary[23]. Sometimes, post-void residual urine volume is measured using ultrasound. The goal is to rule out or treat organic causes (infection, enlarged prostate, tumors, neurological diseases)[24]. If a correctable cause is identified (e.g., urinary tract infection), it is treated first with antibiotics or appropriate therapy.
When should you see a specialist? Depending on the case, this could be a urologist (for men) or a urogynecologist or pelvic floor physical therapist (for women). You may also want to see a psychologist or sexologist if emotional factors play a major role. It is especially recommended to seek help if initial strategies (dietary changes, pelvic exercises) do not improve symptoms, or if incontinence occurs after surgery or following childbirth. As Cigna advises: “If you have symptoms of urinary incontinence, don’t be embarrassed to tell your doctor”[18]; early evaluation leads to better outcomes. At our center in Palma, we offer multidisciplinary teams (urology, gynecology, physical therapy, psychology/sexology) for this integrated diagnosis and treatment.
Management and prevention strategies
Effective management of incontinence combines physical and mental treatments:
- Pelvic floor physical therapy: This forms the basis of behavioral treatment. It includes strengthening exercises (Kegels) to improve bladder support[25]. The doctor usually prescribes at least three daily sets of pelvic floor contractions (holding for 5–10 seconds each time)[26], often with biofeedback or electrostimulation to ensure proper technique. Stress incontinence, in particular, improves significantly with this training.
- Behavioral techniques: Bladder training (gradually delaying urination), a fixed urination schedule (going to the bathroom every 3–4 hours even if there is no urge), fluid management (limiting caffeine and alcohol), and healthy bowel habits (avoiding constipation)[27][28]. Simple changes are also recommended: easy-to-use bathroom facilities, ensuring the bathroom is accessible, and avoiding known triggers. These measures can significantly reduce leakage.
- Relaxation and stress management: Given the impact of emotions, techniques such as deep breathing, progressive muscle relaxation, and mindfulness are helpful. For example, taking a few slow breaths while visualizing the pelvic floor lowering as you exhale releases accumulated tension[29][20]. Studies show that daily practice of relaxation and mindfulness reduces pelvic hyperreactivity and urgency episodes[20]. The Mayo Clinic’s recommendations for stress include meditation and breathing exercises[20]. You can start with 5–10 minutes of guided meditation daily (free apps) or body scan meditation. The image above illustrates an outdoor meditation scene, which helps reconnect the body and mind[20].
- Psychological or sex therapy: Cognitive-behavioral therapy (CBT) helps manage anxiety, change catastrophic thoughts, and reduce excessive focus on symptoms. A psychologist also teaches gradual exposure techniques: e.g., calmly imagining emergency situations and practicing strategies (breathing, pelvic relaxation) as described above[20]. In cases of relationship dysfunction (mutual blame, lack of communication), couples or sex therapy helps open up dialogue and foster mutual support.
- Healthy lifestyle: Maintaining a healthy weight reduces pressure on the bladder (excess abdominal weight is a risk factor[5]). Avoid tobacco (chronic coughing worsens stress incontinence) and regulate fluid intake (do not restrict fluids too much, but avoid drinking too much before bedtime). Regular aerobic exercise (walking, swimming, yoga) improves circulation and overall muscle tone, which can alleviate incontinence in the medium term.
- Practical examples: Simple exercises can be done at home: while lying down, contract your pelvic floor muscles as if you were stopping the flow of urine, hold for 5 seconds, and relax for another 5 seconds[26]. Another option is to perform the exercise in more challenging positions (standing, sitting cross-legged). For urge incontinence , the “delay technique” is recommended : when the urge arises, take 10 slow breaths before going to the bathroom, repeating this every time you feel the urge, until you are able to delay the urge. These habits, when practiced consistently, help “reset” the body’s response to stress.
Communication and Overcoming Shame
Talking openly can be a relief. Sharing your concerns with your partner, family members, or trusted friends can often help alleviate feelings of loneliness and guilt. In a medical setting, remember that healthcare professionals (urologists, gynecologists, nurses, and sexologists) routinely treat incontinence without judgment. It is recommended not to put off seeking medical advice out of embarrassment: experience shows that people often feel better after expressing their concerns[18].
To facilitate communication between partners, small changes are suggested: for example, agreeing together on intimacy routines that don’t cause anxiety (physical closeness without immediate sexual pressure), or using humor to ease tension. In sex therapy or psychological counseling, body image is often addressed: the pelvic floor is not “to blame” for the loss, but rather a muscle that needs support. Learning together about the causes of incontinence helps reduce irrational fear. Finally, community resources (support groups, sex education workshops) can be helpful for sharing experiences.
Additional resources and referrals
In summary, a comprehensive approach to incontinence includes:
- Referral to specialists: urology (for men) or gynecology (for women) to rule out medical causes and consider treatments such as medication or surgery in advanced cases.
- Pelvic floor physical therapy: As a first-line, non-invasive treatment. In Palma, we have specialized physical therapists who teach pelvic floor exercises and relaxation techniques.
- Psychological or sex therapy: Psychologists and clinicians specializing in sexual health to address stress, guilt, and interpersonal communication.
- Health education: Nurses and social workers can provide guidance on lifestyle habits (diet, bladder care) and refer patients to self-help groups or local workshops.
In addition, there are clinical guidelines (from the Spanish Society of Urology, the Spanish Society of Gynecology, and regional health guidelines) and educational materials (brochures, sexual health websites) that explain incontinence and its treatment. At our center in Palma, we have integrated these resources to provide comprehensive care.
Conclusion
Urinary incontinence is not just an isolated physical problem, but a multifaceted condition. The mind-body connection means that emotions such as stress, anxiety, shame, or fear have a direct impact on bladder control. Recognizing this connection allows for more effective treatment: combining pelvic physical therapy with emotional management and lifestyle changes. Don’t ignore the signs: seeking help can significantly improve your health and well-being. In practical terms: strengthen your pelvic floor with exercises, train your bladder with discipline, learn to relax through mindful breathing, and maintain a healthy routine. With professional support and a holistic approach, it is possible to overcome incontinence and regain peace of mind, self-confidence, and full intimacy.
The information in this article is based on current clinical guidelines and clinical studies (urology and gynecology societies, the Mayo Clinic, and recent research) to provide a scientific and practical overview of this issue, without replacing a personalized medical consultation.
[1] The Pelvic Floor and Emotions
https://www.suelopelvicovalencia.es/suelo-pelvico-y-emociones
[2] [3] [5] [6] [7] [9] [10] [11] [12] [22] [24] Urinary incontinence – Symptoms and causes – Mayo Clinic
https://www.mayoclinic.org/es/diseases-conditions/urinary-incontinence/symptoms-causes/syc-20352808
[4] [8] [18] Urinary incontinence in women | Cigna
[13] [14] [15] [20] [21] [29] Anxiety and the Pelvic Floor: How to Break the Vicious Cycle
[16] [17] Depression and Anxiety in Women with Urinary Incontinence: Assessing Their Quality of Life – Dialnet
https://dialnet.unirioja.es/servlet/articulo?codigo=10590446
[19] Somatic Symptom Disorder: MedlinePlus Medical Encyclopedia
https://medlineplus.gov/spanish/ency/article/000955.htm
[23] [25] [26] [27] [28] Urinary incontinence – Diagnosis and treatment – Mayo Clinic